I’m writing from experience. Not from following the low FODMAP diet for myself, but doing it for my 16-year-old daughter. This means I am living and breathing it and cooking or preparing FODMAP friendly meals. This has been a challenge. As a nutritionist it goes against everything I believe in and are taught about nutrition and packing my family’s diet with all different fruits and vegetables, wholegrain bread and pasta, beans and pulses.
My daughter for some time has suffered from unexplained bloating and gas, she has had every test under the sun, but all came back negative, although she has mild IBS (irritable bowel syndrome). The only course of action left to try to find out what was causing her symptoms was to try the low FODMAP diet. But what is this diet and how do you follow it?
What does FODMAP mean?
FODMAP is an abbreviation for
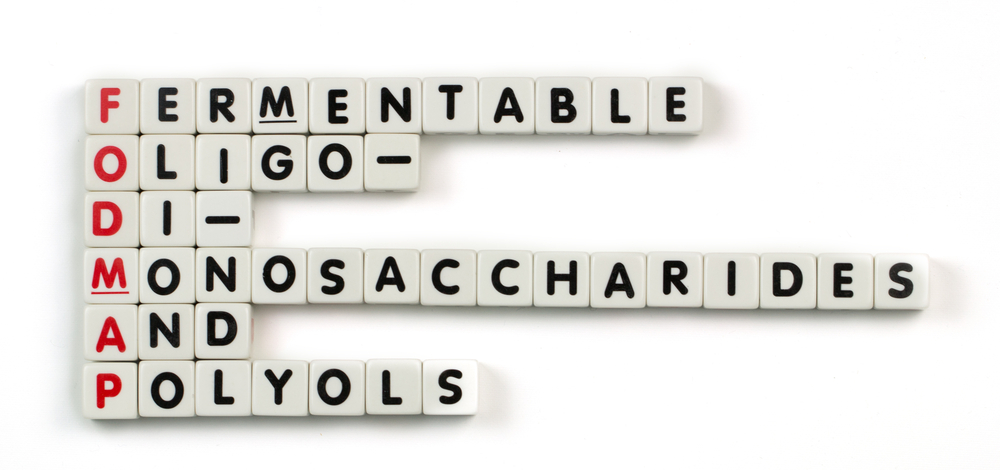
. It is believed that some specific foodstuffs are dietary triggers for symptoms of bloating, gas, stomach discomfort, constipation and diarrhoea, and other symptoms of IBS. FODMAPs are fermentable carbohydrates. This means that when these certain carbohydrates are eaten, they can have a tendency to ferment in the gut and causes bloating etc. The fermentation usually occurs in the large bowel as gut bacteria consume these FODMAP carbohydrates, the gases produced from fermentation are usually the cause of the bloating and discomfort.
The low FODMAP diet is a way to try to identify which (if any) particular fermentable carbohydrates trigger the gut to produce gas and discomfort. It might be that only one or two particular carbohydrates cause the worst symptoms and therefore an individual can then choose to limit or omit these foodstuffs from their daily diet. Omitting all of these FODMAPs though is not considered to be a long term solution and should not be adopted full time. The diet should only be used to identify which particular foods are triggers, and to omit or reduce consumption of these.
Which carbohydrates are considered as FODMAPs?
Fructans are chains of sugar fructose and common food sources are; wheat and rye, various fruit and vegetables, and so called ‘prebiotics,’ these are insoluble fibre that ‘feed’ our gut bacteria such as inulin.
Galacto-oligosaccharides (GOS) are foodstuffs such as pulses and legumes e.g. chickpeas, lentils, beans. These carbohydrates are difficult to break down and absorb in all individuals, but some struggle more than others and the gas produced by bacteria digesting these molecules causes the discomfort experienced by IBS sufferers, for instance.
Polyols tend to be used in sugar free foodstuffs to add low calorie sweetness. If a product contains them you can see on the label – sorbitol, xylitol or mannitol. They are also found in some fruit and vegetables.
Fructose is a monosaccharide and contained in various fruit and fruit juices as well as honey and agave nectar
Lactose is found in milk and yoghurt
How does the diet work?
If for any reason you feel you should try this diet because of unexplained bloating and discomfort it is important that you consult your GP first to rule out any other potential causes of your symptoms and then ask for a referral to a dietitian. It is recommended that if you follow the low FODMAP diet it should be dietitian supervised. It is not recommended to follow this diet without supervision and support.
That said, I’d like to explain a little more about what the low FODMAP diet involves and the challenges I have faced with my daughter along the way. The first phase of the low FODMAP diet is to eliminate all the FODMAP foods from your diet for 6-8 weeks. This is difficult, because many day to day foods contain one or more FODMAP ingredients. Wheat for example is an ingredient found not just in bread, but biscuits, cakes, sauces, pasta, noodles, pastry, breakfast cereals, breadcrumbs and batter. If you regularly eat fruit and vegetables, then many common types such as apples, pears, sultanas, onions, garlic, cauliflower, mushrooms must all be avoided and replaced with low FODMAP types such as grapes, oranges, pineapple, strawberries, broccoli, carrots, courgettes and green beans. Normal milk, must be swapped for lactose free or nut, oat or rice milks. Yoghurt, ice cream, milk chocolate and custard should all be avoided. Legumes must all be avoided, so if you like lentils, chickpeas and beans, then you must eliminate these for the first 6-8 weeks.
After the elimination phase is completed then if you are susceptible to bloating and discomfort from FODMAPs, then you should start to feel a little better. Phase two involves a gradual reintroduction of each FODMAP type, even down to individual foodstuffs. This process can equally take up to 6-8 weeks, depending on how many individual products you decide to re-introduce. The intention of this phase it to pinpoint any foodstuffs that cause a reaction in the gut i.e. make you feel bloated and uncomfortable. If you are able to identify any particular foodstuffs, then you can choose to eliminate this or reduce their consumption from your day to day diet and have some control over how you feel.
Challenges
As you can imagine this is a very difficult diet to follow, hence you need support from a dietitian. A lot of time is spent preparing meals well in advance and having a very specific shopping list. If you are trying to cook for a family and one individual is following the low FODMAP diet, then this can be challenging but not impossible. You can adapt some meals and there are some very good cookbooks for ‘real’ meals that the whole family can enjoy.
I found that wheat free bread was not very appetising and difficult to work with in terms of making a sandwich for example, so I found that avoiding bread for my daughter was easier than trying to use a wheat free bread. When it came to batters and coatings, you can easily buy simple wheat free coated fish and chicken that tastes good, so I used these. Wheat free and FODMAP friendly biscuits and treats can be found in the supermarket, but requires a bit of label reading to find the right ones. Using ‘allowed’ fruit and vegetables was quite easy to manage, but after 8 weeks became a little monotonous. I like to be inventive with my cooking, but I found this difficult, because many ingredients contain a variety of FODMAPS, so it’s easier to stick to basic meals of protein, vegetables and potatoes or rice for instance.

I do think this diet would be more challenging for a vegetarian or vegan, mainly due to the limitation on allowed vegetables and the restrictions of the use of legumes, as these are staples for a meat free diet. That said, it’s not impossible. The use of lactose free milk was preferred by my daughter than nut, oat or rice milk, mainly because the taste is not too different to normal milk. Orange juice was swapped for cranberry juice, milk chocolate for high cacao chocolate.
A big challenge was not being able to use garlic, onions and leeks, as these are staple ingredients for many sauces, soups, gravy, meals etc. I made a lot of homemade sauces without these ingredients and substituted in ‘allowed’ herbs and spices. Homemade tomato sauce on wheat free pasta was a popular meal.
Considerations
A diet that limits certain fruits and vegetables, wheat and rye, and legumes limits fibre intake. In the UK we should be eating at least 30 g of fibre per day. By not meeting this target an individual can suffer from bloating and constipation, also symptoms of FODMAP sensitivity. This is a good reason why the low FODMAP diet is not a long term solution and should only be followed to identify particular trigger foods and limit their consumption.
Lactose free milk contains less vitamin B12 and calcium than say standard semi skimmed milk, but still has a similar nutrient profile. However, nut, oat and rice drinks are not as diverse in their nutrient profile as dairy milk and as such anyone switching to these types, should be aware that they choose fortified versions, or consider supplements in calcium and B12 if they have no other food source in their diet.
Research investigating this diet
A study at King’s College London (2019) found that a diet low in fermented carbohydrates improved certain gut symptoms and health-related quality of life for sufferers of irritable bowel disease. After four weeks on a low FODMAP diet patients who were experiencing persistent gut symptoms prior to the four weeks had improved symptoms of stomach swelling and flatulence afterwards.
A study by the University of Otago in New Zealand (2019), found that the low FODMAP diet was a useful treatment for children and adolescents (aged between 4-17) with gastrointestinal problems. The study found that after completion of the diet 92% of children (total in the study was 29) with bloating, 87% with diarrhoea and 77% with abdominal pain had complete resolution of gastrointestinal problems. In the re-introduction phase fructans were found to be the main cause of intolerance at 67%, followed by lactose (56%), polyols (7%) and fructose (7%). Six children found that apples triggered their gastrointestinal problems.
However, a report looking at the controversies and recent developments of the low FODMAP diet by Hill, Muir and Gibson (2017), identified that there have been very few large scale studies on the effects of the low FODMAP diet on people and children with gastrointestinal issues. They also identified that the diet carried risks of low nutrient intake and encouraged disordered eating, and caused potentially unfavourable gut microbiota. It could be argued that due to these risks, it’s important that anybody undertaking this diet is supported and supervised by a qualified dietitian.
So what about my daughter?
We’ve completed the 6 weeks of total FODMAP elimination and she feels a little better, but not dramatically so, although when we started she did feel a little better than some months ago when she felt bloated and uncomfortable. We are now in week three of the re-introduction phase. First we reintroduced wheat very slowly, from a slice of white bread each day for three days to two slices or a slice in the morning and a small portion of pasta in the afternoon for another three days. She felt no noticeable gut problems. We are now trying garlic and next week we will try onions and leeks. We will continue this way until we have covered all the main FODMAPs. She wants to try milk next as she is desperate to get back to eating ice cream!
What have I learnt from this? Well FODMAPs might not be the cause of her issues. Maybe it’s been the stress of exams or teenage hormones. We will discuss this further with the dietitian. But I have learnt a lot more about these so called FODMAPs and maybe some people who blame gluten for their issues, might actually have an intolerance to fructans. We also need to see more research in this area, with larger groups of participants. I would certainly support this.
References
Hill, P., Muir, J. G., Gibson, P. R. (2017) Controversies and Recent Developments of the Low-FODMAP Diet. Gastroenterology & Hepatology. Vol 13, Issue 1.
King's College London. (2019, October 3). FODMAPs diet relieves symptoms of inflammatory bowel disease. ScienceDaily. Retrieved October 17, 2019 from www.sciencedaily.com/releases/2019/10/191003173744.htm
University of Otago. (2019, September 24). Benefits and safety of FODMAP diet in children. ScienceDaily. Retrieved October 17, 2019 from www.sciencedaily.com/releases/2019/09/190924101440.htm